Artificial Intelligence (AI): After the Dental Implant
Artificial Intelligence (AI): After the Dental Implant
Artificial Intelligence can now define diseased dental implant outcomes.
The term science fiction is literally a hundred years old; it’s concept however, is almost four hundred.
Published in 1638 The Man in the Moone is a novel by Church of England bishop Francis Godwin. An explorer builds a space ship and meets “people most strange,” on another planet. They’re twice as tall as humans, and wear clothes of a mysterious material. Its dye is a colour unseen by human eyes, and they speak in haunting musical tones. Its 17th century audience was captivated by its tale of a Spaniard whose ship is powered by geese. He flies through space; which for the first time in literature is depicted as weightless. He spends time with the citizens of a lunar civilisation, then returns to Earth to an exotic and technologically marvellous land called China.
It’s an exploration plot of countless examples: from Asimov to Adams; from 2001: A Space Odyssey to Interstellar.
The happenings in the reality of AI over the last two decades are as spectacular as if that medieval reader had finished reading The Man in the Moone then trotted off to the cinema to see Star Wars.
Growth and development in the field of artificial intelligence (AI) in health care research has lead to its expansion into areas once considered the exclusive reserve of humans. AI applications are becoming expert in data acquisition, learning and computing infrastructure: building the hardware and systems for other processes and services.
Applied to medicine and dentistry, AI holds remarkable potential for revolutionising the health industry and refining patient care.
In dentistry, AI is being researched and explored specifically for the identification of normal and abnormal structures, streamlined diagnosis, and prediction of treatment outcomes.
Artificial intelligence is an exponential technology that has apparatus performing tasks once restricted to having to be done by humans. Advances give a glimpse of health care benefits, such as improving the process of treatment decisions, eliminating unnecessary procedures, and minimising postoperative complications.
All of it positively impacts on quality of life with fewer interventions, diagnosis accuracy, and more assured prognosis and recovery programme. It plays a crucial role in revolutionising the entire realm of health care and how it is viewed.
It is used extensively in dental laboratories, and is finding a pivotal place in the education and teaching of dental issues, treatments and techniques.
The computer science of AI endeavours to understand, create and design intelligent entities, most of which are exemplified as software programs, defined as a sequence of operations to perform a specific task.
Historically, artificially intelligent systems applied specific rules to the tasks they were to solve, requiring knowledge, engineering and fine-tuning by subject-matter experts. An example would be a system designed to detect lesions in medical imaging that looks for abnormally coloured lumps of a given shape. Fine-tuning might be the range of healthy tissue colours, or minimum dimensions in identifying a potential lump.
Now, a branch of AI known as machine learning and, more recently, deep learning is most commonly used.
Machine Learning (ML) is where a system learns intelligent performance without prior information or handcrafted rules. Without human assistance, it instead identifies patterns in examples from a large dataset by defining an objective, and optimising function to achieve it. This process, known as training, has an ML algorithm exposed to random examples to gain experience, and gradual adjustments are made until the wanted outcome occurs. As a result, the algorithm identifies patterns in the same way a child can be shown pictures and photographs of an elephant to learn the pattern of recognition and apply it to new images.
Deep learning imitates the way humans gain certain types of knowledge. While machine learning algorithms are linear, deep learning algorithms are stacked in a hierarchy of increasing complexity and abstraction. Much like that elephant-identifying kid learning that a white elephant, a pink elephant and an elephant in the room are indeed elephants, and at the same time, absolutely not at all.
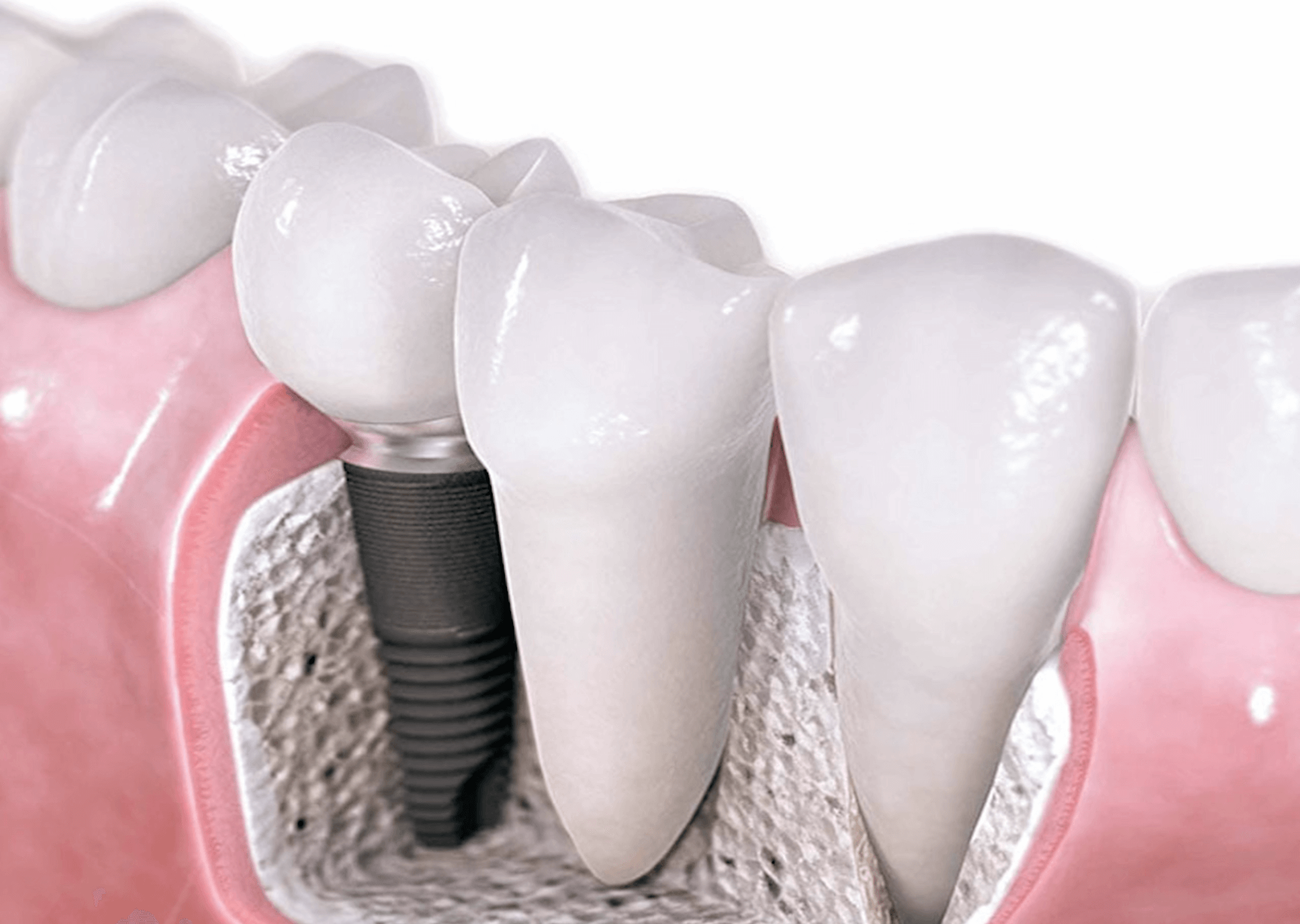
Dental implants and crowns, because of their aesthetic function and natural feel, is a market estimated to reach $6.8 billion by 2024. Implants have transformed reconstructive dentistry, but the emerging endemic of peri-implantitis has severely compromised the long-term success of implant surgery.
Peri-implantitis is an infection of tissue and bone around dental implants that affects roughly 25% of patients, and there has never been a reliable way to assess a patient’s response to treatment.
The condition can lead to progressive bone loss, bleeding, chronic infection and eventual loss of the implant, and the relative crown or dentures it supports. Replacement implants are challenging because of poor bone quality and delayed healing. Expensive long-term preventive maintenance and management of peri-implantitis is routine practice after implant reconstruction and outcomes are unpredictable.
A team led by the University of Michigan School of Dentistry developed a machine learning algorithm to assess an individual patient’s risk of regenerative outcomes after surgical treatments of peri-implantitis.
Called FARDEEP (Fast and Robust Deconvolution of Expression Profiles) it analysed tissue samples reconstructive therapy patients. They quantified the profusion of harmful bacteria and infection fighting immune cells in each sample.
Patients at low risk for periodontal disease showed types of immune cells that were highly adept at controlling bacterial infection. The team was surprised to find that there are cells associated with better outcomes for implant patients that challenged conventional thinking.
Prior to their discovery, much emphasis had been placed on immune cell types that are more adept at wound healing and tissue repair, and here was evidence of immune cell types central to microbial control, and strongly correlated with superior clinical outcomes.
Surgical management reduces bacterial burden across all patients; however, only patients with more immune cell subtypes for bacterial control can suppress the recolonisation of pathogenic bacteria. This is what gives them a much better regenerative outcome.
Soon it will be possible to predict the risk of peri-implantitis before a dental implant, with more human clinical trials are required before FARDEEP can be widely used by clinicians in determining the best course of treatment between replacing the implant despite the challenge to rebuild the bone, or regenerative therapy knowing it would be successful.
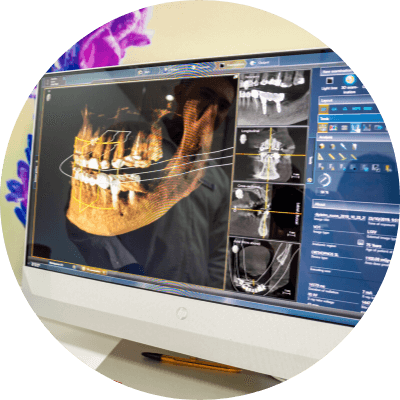
Amid these incredible advances, another team of researchers at the Finnish Center for Artificial Intelligence (FCAI), with high-tech dental equipment manufacturer Planmeca, and the Alan Turing Institute have successfully developed a new model for locating mandibular canals; fundamentally minimising the risk of nerve damage in dental implant surgery.
A dentist must know the precise location of the mandibular canal in order to plan dental implant surgery: damage or lesions to the inferior alveolar nerve causes pain and variations to sensitivity in the patient’s lower jaw; and a tingling or burning sensation known as paraesthesia occurs with damage to peripheral nerves.
In a small number of cases it will remain a permanent condition; for others, up to six months, with the majority recovering in a matter of days or weeks.
For although mandibular molars tend to have similar root canal configurations, there are several atypical variations.
These variations are the difference between the implant failing, and attaining optimal clinical outcomes.
Based on the research results, the deep learning model is highly accurate in locating the mandibular canals highly accurately, surpassing the statistical shape model – the best, automated method until now.
In more complex cases, the estimate may need small adjustments, so it’s not a complete stand-alone system yet.
Although multiple studies show the potential of AI in dentistry, the systems are far from being able to replace dental professionals, and successful integration of AI requires specialised training for which most institutions are not currently prepared.
With its great advantage of rapidity and precision every time, Artificial Intelligence is a complementary assistance asset for dentists and specialists. Its safe and regulated integration retains the role of dentists directing treatments, and continuing to make informed decisions across the many aspects of oral health and dentistry.
The aim of this research work is not to replace oral health care professionals, but to make treatments and procedures more efficient. AI gives more time and greater confidence for the dentist to focus on the task while observing the state of their patient throughout each stage of the most complex procedures.
One day, Artificial Intelligence won’t be artificial. It may just be called “intelligence” by then.
DISCLAIMER:
The content has been made available for informational and educational purposes only. Melton Dental House does not make any representation or warranties with respect to the accuracy, applicability, fitness, or completeness of the content.
The content is not intended to be a substitute for professional personal diagnosis or treatment. Always seek the advice of your dentist or another qualified health provider with any questions you may have regarding a dental or medical condition. Never disregard professional advice or delay seeking it because of something you have read or seen on the Site.
Services we mentioned:
More Wellness Infographics
Red, Red Wine: Is It Beneficial For Oral Health?
Is red, red wine beneficial for our oral health? Or does it just feel good at the time & if you overdo it you feel like cr*p the next morning…
Detecting Oral Cancer Is Given The Brush
In 2020, Oral Cancer accounted for almost 380,000 cases, and 180,000 deaths globally. It’s on the increase with diagnosis incidents…
Could The Surge In Pneumonia In Children Be Related To Their Teeth Brushing?
Kids and teenagers are not self-maintaining, and nor is their oral health. Teeth brushing: spend time with it frequently…
What Is Dental Sleep Medicine? It’s Not Sleep Dentistry
Dental Sleep Medicine is the intersection of dentistry with issues affecting sleep. Snoring, sleep apnoea, & related breathing disorders…